The Coronavirus might have been spreading quietly in humans for years, or even decades, without causing a detectable outbreak. Dr. Francis Collins, Director, The National Institutes of Health.
Some history: When Swine Flu struck during the 1976 presidential campaign, Gerald Ford endorsed mass immunization, but the vaccine proved both ineffectual and lethal, and contributed to Ford’s loss. When AIDS struck five years later, Ronald Reagan ignored it and was reelected in a landslide.
It is no wonder that our governments treat epidemics as acts of a capricious God–as they have done every ‘flu season for centuries. Says UK Opposition Leader Jeremy Corbyn, “I distinctly remember going to a meeting at the Cabinet Office, where we got a lecture about herd immunity. The last time I discussed herd immunity was when I worked on a pig farm 40 years ago. It was absurd that actually you would build up herd immunity by allowing people to die. And so, while the government was going into eugenic formulas and discussing all this stuff, they were not making adequate preparations.”
When the WHO announced the Covid-19 outbreak in January, 2020, the CDC’s Dr. Fauci announced, “The American public shouldn’t worry about the coronavirus outbreak in China”. The CDC, born in 1946 as the US Army’s Communicable Disease Center and headed by a non-scientist Army officer, has always provided surveillance, research, and advice, leaving execution to the Army’s chain-of-command. Finland’s Institute for Health and Welfare probably fields more public health staff than the CDC.
The White House first ignored the WHO, then classified discussions, moved them to secure facilities, and released information on a need to know basis. The CDC banned Covid testing and served recalcitrant officials with cease and desist orders. Only after the 2020 election did thirty-four CDC researchers, using archived Red Cross blood samples, announce what many had suspected: by December, 2019, the virus was well established in the USA.
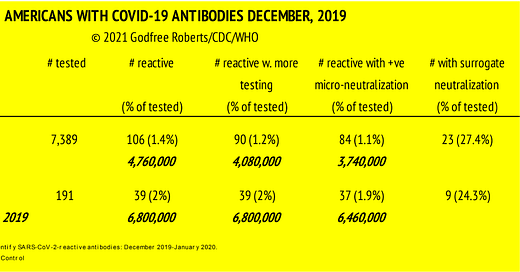
Findings: Of the 7389 samples, 106 were reactive by pan-Ig. Of these 106 specimens, 90 were available for further testing. Eighty-four of 90 had neutralizing activity, 1 had S1 binding activity, and 1 had receptor-binding domain/ACE2 blocking activity >50%, suggesting the presence of anti–SARS-CoV-2–reactive antibodies. Donations with reactivity occurred in all 9 states.
Conclusions: These findings suggest that SARS-CoV-2 may have been introduced into the United States prior to 19 January 2020.
a study from researchers at Washington University School of Medicine in St. Louis found that, months after recovering from mild cases of COVID-19, people still have immune cells in their body pumping out antibodies against the virus that causes COVID-19, according to Such cells could persist for a lifetime, churning out antibodies all the while.[SARS-CoV-2 infection induces long-lived bone marrow plasma cells in humans. Turner, J.S., Kim, et al. Nature, May 24, 2021]
The obvious question is: howlongbefore 19 January 2020 was SARS-Cov-2 introduced?
Happily, the answer is not far to seek.
If we know the death doubling interval–how long it takes for the number of total confirmed deaths to double in America–and the number of one month’s confirmed Covid deaths, we can calculate the approximate date when the virus started killing us.
It takes one-hundred thirty-nine days for Covid deaths to double in the US, and 70,000 Americans died of Covid in January 2020. Working backwards, and halving the deaths every 139 days, we find that the virus appeared here around 2015.
The date is supported by similar findings from Europe, especially from an Italian research team:
Abstract: SARS-CoV-2 RBD-specific antibodies were detected in 111 of 959 (11.6%) individuals, starting from September 2019 (14%), with a cluster of positive cases (>30%) in the second week of February 2020 and the highest number (53.2%) in Lombardy.
Conclusions: People with no symptoms not only were positive after the serological tests but had also antibodies able to kill the virus. This means that the new coronavirus can circulate among the population for long and with a low rate of lethality not because it is disappearing, but only to surge again”.
Why did we not detect it? A clinician friend explained,
The argument that Covid-19, if already spreading in the US, even in 2019, would have been mandatorily detected in real-time just because of an alarming quantitative increase in the death rate is obviously wrong. If that were the case, the Italian and Spanish Health services who struggled for four months with high concentrations of elderly Covid-19 patients would have seen such an “excess mortality” red flag, but they never did, until the Chinese made a decisive qualitativestep forward and identified a novel virus.
Covid has a low death rate, and as such could not have been identified just by an alarmingly-increased excess death rate, especially in the early months of the pandemic when the number of cases were low. It is the qualitative factors, clinical symptoms, scans, serology, and the like that should have raised the red flag, but instead the CDC chose to bury them under the now-discredited “EVALI” convenience tag.
The Chinese identified SARS-CoV2 led by qualitativedrives, not because they had too many deaths, but because they reacted as perfectionist professionals when faced with symptoms they could not attribute to any previously-known respiratory syndrome.
It would have been extremely easy to hide the statistical effect of 6 - 7 months of running Covid19 infection in the USA, especially at the inception stage of the epidemic. Laymen may object that, if 100,000 died, someone would have noticed. No.
Maybe somebody would have “noticed” an extra 100,000 deaths, but not until they had accumulated and been totalised alongside the excess death or negative death rates from all other factors. For instance, the uncertainty on the death toll for ‘flu during only the 6-months winter season is as high as 38,000 deaths–so it would have taken a long time for an extra 100,000 deaths to raise a red flag as a confirmed anomaly.
In other words, considering its comparatively small order of magnitude, the 2019 Covid death rate would have been easily missed amongst other uncertainty factors such as ‘flu death rate and falling life expectancy.
Finally, it now appears that China, far from being the source of the outbreak, may have been the last to experience it, since the WHO found no evidence of Covid there before December, 2019. The statistics, and the country’s quick response, support that conclusion:
Godfree Roberts is the author ofWhy China Leads the World: Talent at the Top, Data in the Middle, Democracy at the Bottom, and publishes the weekly newsletter, Here Comes China.
REFERENCES
Evidence of early circulation of SARS-CoV-2 in France: findings from the population-based “CONSTANCES” cohort.Fabrice Carrat, Julie Figoni, Joseph Henny, Jean-Claude Desenclos, Sofiane Kab, Xavier de Lamballerie & Marie Zins European Journal of Epidemiology Abstract: Using serum samples routinely collected in 9144 adults from a French general population-based cohort, we identified 353 participants with a positive anti-SARS-CoV-2 IgG test, among whom 13 were sampled between November 2019 and January 2020 and were confirmed by neutralizing antibodies testing. Investigations in 11 of these participants revealed experience of symptoms possibly related to a SARS-CoV-2 infection or situations at risk of potential SARS-CoV-2 exposure. This suggests early circulation of SARS-CoV-2 in Europe. https://doi.org/10.1007/s10654-020-00716-2
SARS-CoV-2 was already spreading in France in late December 2019. A. Deslandesa V.Bertia Y.Tandjaoui-Lambotte bc ChakibAllouia E.CarbonnelleadJ.R.ZaharadS.BrichleraYvesCohenbe Show more Share Cite https://doi.org/10.1016/j.ijantimicag.2020.106006Get rights and content Highlights • SARS-CoV-2 was already spreading in France in late December 2019, 1 month before the first official cases in the country. • Early community spreading changes our knowledge of the COVID-19 epidemic. • This new case changes our understanding of the epidemic, and modelling studies should adjust to these new data. Abstract The COVID-19 epidemic is believed to have started in late January 2020 in France. Here we report a case of a patient hospitalised in December 2019 in an intensive care unit in a hospital in the north of Paris for haemoptysis with no aetiological diagnosis. RT-PCR was performed retrospectively on the stored respiratory sample and confirmed the diagnosis of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection. Based on this result, it appears that the COVID-19 epidemic started much earlier in France.